What is an implantable port and why does it transform pediatric cancer care?
Every year, around 400,000 children worldwide are diagnosed with cancer. Childhood cancers require aggressive chemotherapy and intensive supportive care. For these demanding treatments, reliable central venous access becomes essential, and implantable ports play a crucial role. (1)
An implantable port is a totally subcutaneous central venous access device that provides stable, repeated entry to a major vein, allowing safe administration of chemotherapy, parenteral nutrition, blood transfer and antibiotics with minimized discomfort. (1)
Why it is indispensable in pediatric oncology:
- Provides essential access to intensive chemotherapy. Ports are described as a cornerstone of supportive care, enabling repeated infusions and blood sampling that peripheral lines cannot safely sustain. (1)
- Protects fragile pediatric veins. Children’s veins are thin and easily damaged, making longterm peripheral access impractical; implantable ports are considered the best option for chronic venous needs. (1) (2)
- Supports multiple therapies through a single device. Ports allow chemotherapy, transfusions, antibiotics, fluid therapy, and blood sampling through one subcutaneous access point, reducing procedural burden. (1)
- Improves comfort and reduces needle trauma. By eliminating repeated venipunctures, ports significantly decrease pain and improve cooperation and overall treatment experience for children. (7)
- Reliable safety profile. Infection and catheter malfunction are the most common complications, yet overall complication rates remain low and manageable when the device is properly maintained (6). Complication rates around 9-10%, with infection at 3.13% and malfunction/obstruction at 3.13% in lower‑incidence settings. (1) (3)
- Adaptable from infancy to adolescence. Ports have been successfully implanted in patients ranging from a few months old to late adolescence, supporting long, complex oncology journeys. (1)
When is an implantable port indicated in pediatrics:
- Planned longterm or cyclical chemotherapy requiring central venous delivery, particularly for vesicant or irritant drugs that cannot be safely administered peripherally. (1) (2)
- A high frequency of venous access needs, including repeated blood sampling, transfusions, prolonged intravenous antibiotics, hydration, or nutritional support. (1)
- Difficulty obtaining or maintaining peripheral venous access because of small caliber, easily compromised pediatric veins or limited tolerance for repeated cannulation. (1)
- Treatment courses extending over months or years, where a fully implanted, low maintenance device improves continuity and comfort.
How do implantable ports compare to other central venous access devices?
Implantable ports (PORTs) show lower infection and complication rates, longer device survival, and fewer premature removals than tunnelled CVCs, while CVCs remain useful mainly for short term high frequency access.
Key differences:
- Intended duration: Centrally inserted CVCs are typically used for 5-7 days (emergency, ICU).
- External vs. internal system: Tunnelled CVCs allow needle‑free access but have an external segment, increasing infection risk and daily maintenance needs. Ports are fully internal, offering better cosmetics and allowing children to continue their usual daily activities without major restrictions. (7)
- Infection risk: Tunnelled CVCs carry significantly higher systemic infection, while PORTs show lower infection incidence than both CVCs and PICCs.
- Mechanical complications: Mechanical failure is also more common in tunnelled CVCs compared with PORTs. (2)
- Premature removal: Removal for complications is over three times more likely in tunnelled CVCs.
What advantages do implantable ports offer over other devices?
PORTs are more cost effective, safer in the long term, easier to maintain, and strongly preferred by families.
Key advantages:
- Cost effectiveness: PORTs cost £210 per catheter‑week, compared with £257 for tunnelled CVCs, and although ports can have a higher upfront cost, their longer lifespan and lower complication rates make them more cost‑effective over the long term.
- Lower complication burden: ports report infection rates around 27% and mechanical complication rates between 1-3%, whereas tunneled CVCs experience 15-40% complication‑related removals. (3) (5)
- Longevity: PORTs remain in place significantly longer than tunnelled CVCs.
- Family preference: Parents show a clear preference for PORTs due to appearance, ease of care, and reduced daily restrictions. (7)

How are implantable ports inserted?
Ports are generally inserted under local anesthesia using minimally invasive ultrasound guided techniques performed by pediatric surgeons, anesthesists or interventional radiologists. (1) (7) (8)
Main insertion methods:
- Seldinger percutaneous approach: A safe, effective method that provides reliable access to central vessels. (1) (8)
- Ultrasound guided percutaneous insertion: Less invasive, associated with fewer complications and reduced bleeding. (1) (8)
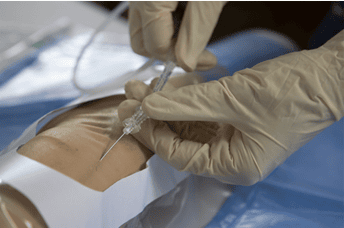
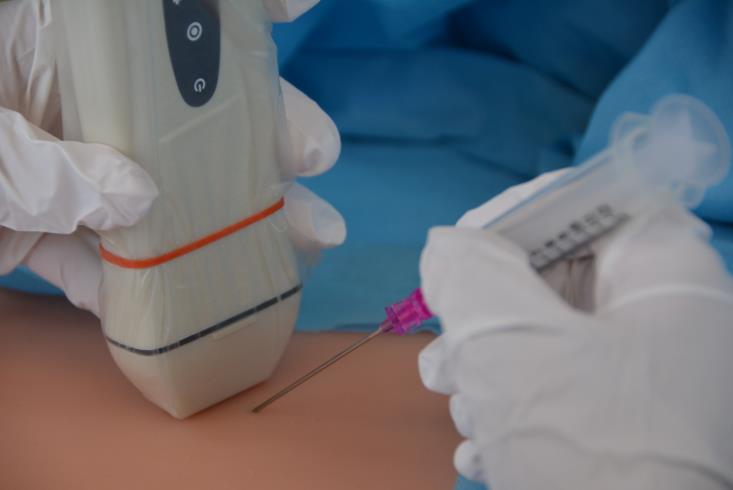
Complications of implantable ports in pediatric oncology and how they can be prevented
What are the mechanical complications?
Mechanical complications are noninfectious device related failures that result from physical, structural, or technical problems with the port system itself. (1)
The most frequent mechanical issues are catheter obstruction/dysfunction, leakage, migration/dislodgement, pneumothorax, hematoma, and pinch off/kinking depending on the access site. (2) (6)
- Obstruction/dysfunction (late): one large cohort documented catheter obstruction in 1.7% of cases and system leakage in 1%. These events reflect intraluminal occlusion, fibrin sheath formation, or catheter damage. (1) (2) (3) (6)
- Migration/dislodgement: reported but less common than infection/obstruction.
- Pneumothorax and pocket hematoma (early): 3% and 2.5% respectively in a large pediatric series. Both are strongly associated with operator experience and the chosen venous access site. (1) (3) (8)
Access site dependent risks:
- Internal jugular vein: Higher risk of malposition, catheter bending, and blockage due to the steeper angle and catheter trajectory. (8)
- Subclavian vein: Susceptible to catheter kinking and pinch off syndrome (compression between clavicle and first rib). (8)
- Brachiocephalic vein: Ultrasound guided BCV access offers higher first attempt success, smoother catheter curvature, and fewer complications, making it increasingly preferred for children. (8)
What are the infectious complications?
Infectious complications are caused by microbial contamination of the port system, including the skin entry site, the subcutaneous pocket, or the intravascular portion of the catheter. Infection is typically the most common overall complication. (1) (2) (6)
- Spectrum and burden: In a single center pediatric cohort of 474 implantations, 27.2% developed infectious complications. Most were late infections and 14% of all implanted children lost their port, accounting for 53% of all infected ports requiring removal. (3)
- Age effect: Children under 5 years old had a significantly higher infection rate than older groups. Early and late infection rates reach 35%, highlighting their higher susceptibility due to smaller vessel size, more challenging care, and greater immune vulnerability. (3) (6)
- Risk vs. alternatives: Tunnelled external CVCs show a 110% higher likelihood of systemic infection compared with implantable ports, and meta‑study summaries report lower infection incidence with PORTs than both tunnelled CVCs and PICCs. (5)
What is the estimated incidence?
Overall complication rates vary by cohort; 9-10% in some pediatric oncology series, but higher in others. Infections and mechanical dysfunction dominate. (6)
- Lower end: In a pediatric cancer cohort, the overall complication rate was 9.38%, primarily driven by infections (3.13%) and catheter malfunction or obstruction (3.13%), supporting the generally favorable safety profile of implantable ports in routine clinical practice.
- A large meta‑analysis including 6,644 devices demonstrates that tunnelled external CVCs are associated with substantially higher rates of systemic infection, mechanical complications, and premature device removal, whereas implantable ports consistently show lower complication rates and better long‑term durability. This finding confirms that most device‑related complications occur with tunnelled CVCs rather than implantable ports, supporting ports as the safer option for long‑term pediatric oncology care.
How can they be prevented?
Outcomes improve with experienced operators, ultrasound guided Seldinger techniques, and standardized asepsis/maintenance, plus targeted anti-infective management when events occur. (2)
- Technique and expertise: The Seldinger method is quick, minimally invasive, and safe. Complications decline as operator experience increases. Ultrasound guided percutaneous approaches reduce bleeding and cosmetic impact. (3)
- Aseptic insertion and care: Rigorous asepsis, trained nursing teams, and standardized dressing/flushing protocols lower infection/malfunction. (2) (6) (7)
- Site selection: Consider brachiocephalic vein access to improve success and lower mechanical risks; avoid subclavian vein kinking where feasible. (5) (8)
- Therapeutic response: Intravenous anti-infective therapy resolves 75% of catheter infections without removal in pediatric series; removal is still necessary in a substantial subset. (3) (6)
Side by side comparison (PORT vs. tunnelled external CVC vs. PICC)
PICCs often serve as temporary access; the pediatric oncology evidence base for longterm comparisons is more limited than PORT vs tunnelled CVC.
| Attribute | Implantable Port (PORT) | Tunnelled external CVC | PICC |
|---|---|---|---|
| Systemic infection risk | Lower; meta-analysis shows lower odds vs tunnelled CVCs | Higher vs PORTs. | Reported higher than PORTs in multicenter observations. |
| Mechanical complications | Lower vs tunnelled CVCs | Higher vs PORTs. | Variable: pediatric oncology data are less robust in direct head to head with PORTs. |
| Premature removal | Lower (fewer removals) | Higher removal rates. | Not directly pooled vs PORTs in pediatric oncology; observational signals suggest more infections than PORTs. |
| Daily care | Low; fully implanted, bathing/swimming allowed. | High; external segment increases maintenance. | Moderate: external line care required. |
| Parent/patient preference | Parents show a clear preference for PORTs; quality of care perceptions positive. | Less preferred due to visibility and care burden. | Mixed: often chosen for short term needs. |
| Costeffectiveness | More cost effective £210 per catheter week. | £257 per catheter week. | Not quantified in these pediatric oncology comparisons. |
| Insertion | OR/IR; GA; Seldinger; ultrasound guided percutaneous cosmetic and low bleeding. | OR/IR; GA; external exit site; frequent handling. | Ward/IR placement; often bedside; for temporary access. |
What is the psychological impact on children and families, and why is education essential?
Childhood cancer carries a significant psychological burden. The presence of a port can create fear, anxiety, or trauma for both children and parents. (9)
Impact and rationale
Children experiencing repeated treatments may suffer from psychological distress, fear of procedures, and heightened anxiety. Parents similarly may experience emotional trauma and uncertainty throughout the treatment journey. Education, reassurance, and continuous communication are essential to mitigate these effects. Examining the psychological impact of childhood cancer (user‑provided info). (9)
Importance of education
Clear explanations of the device, its purpose, and each procedural step help reduce fear, increase cooperation, and support emotional resilience for both the child and the family. (7) (9)
The value of implantable ports in pediatrics
Implantable ports are fully subcutaneous central venous access devices that provide stable, repeatable and safe entry into a major vein, an essential requirement for the intensive chemotherapy and supportive therapies children with cancer frequently need. Their design protects fragile pediatric veins, reduces needle related trauma, and allows multiple treatments to be delivered through a single, reliable access point. (7)
In pediatric care, implantable ports offer several advantages over external central venous catheters. They show lower infection and mechanical complication rates, remain functional for longer periods, and require less daily maintenance. When ports are placed using appropriate techniques such as ultrasound guided percutaneous insertion or the Seldinger method by experienced operators, the risk of complications, particularly infections, is significantly reduced. Consistent aseptic handling and proper maintenance further strengthen their safety throughout treatment.
Beyond clinical performance, implantable ports also support the emotional and practical needs of children and their families (7). Their discreet design, fewer needle punctures and compatibility with normal activities like bathing or swimming help children maintain a sense of normalcy during treatment. Equally important is the guidance provided to children and parents (5). Clear explanations, reassurance and ongoing communication help families cope with fear, uncertainty and stress. When healthcare teams support both the medical and psychological needs of the child and family, implantable ports become not only an effective clinical tool but also a stabilizing companion throughout the pediatric cancer journey. (9)
Bibliography:
- Ghmaird A S, Mohammad Alnoaiji M S, Alalawi Y S, et al. (August 23, 2021) Port-a-Cath Insertion in Pediatric Patients With Malignancy in Tabuk. Cureus 13(8): e17379. DOI 10.7759/cureus.17379
- Esfahani H, Ghorbanpor M, Tanasan A. Implantable Port Devices, Complications and outcome in Pediatric Cancer, a Retrospective Study. Iran J Ped Hematol Oncol. 2016;6(1):1-8. Epub 2016 Mar 15. PMID: 27222696; PMCID: PMC4867165.
- Sosnowska-Sienkiewicz P, Morycin´ ski S, Januszkiewicz-Lewandowska D, Michalik K, Madziar K, Kukfisz A, Zielin´ ska D and Man´ kowski P (2024) Totally implantable venous ports in infants and children: a single-center retrospective study of indications and safety.
- Front. Oncol. 14:1351630. doi: 10.3389/fonc.2024.1351630
- Neville JJ, Aye HM, Hall NJ. Arch Dis Child 2023;108:975–981
- Zhang S, Xiao Z, Yang F. Analysis of related complications of totally implantable venous access ports in children’s chemotherapy—single center experience. Medicine 2022;101:27(e29899).
- Mrs. Menaka Raghuraman. “Port-a- Cath – A friendly partner in the care of child with cancer, A Case presentation.” IOSR Journal of Nursing and Health Science (IOSR-JNHS), 10(2), 2021, pp. 23-30.
- Ding W, Qiu L, Li T, et al. Ultrasound-guided totally implantable venous access ports placement via right brachiocephalic vein in pediatric population: A clinical debut. Pediatr Blood Cancer. 2022;69:e29911. https://doi.org/10.1002/pbc.29911
- American Psychological Association. (2023, October 3). Examining the psychological impact of childhood cancer. https://www.apa.org/topics/children/cancer-psychological-impact