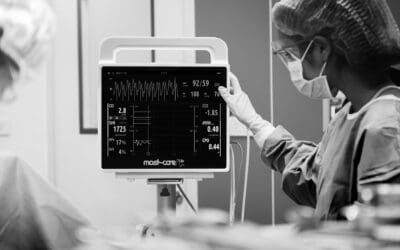
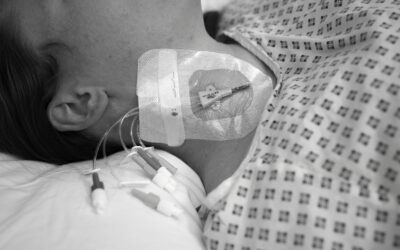
Nurses are the first clinical aid at the bedside, monitoring and responding to changes in patient conditions. Providing nurses with tools to make more informed decisions can significantly enhance patient care as early detection of preventable outcomes is crucial for timely intervention [1,2]. While vital signs provide valuable insights, they often reflect later stages of haemodynamic compromise. As highlighted by Brekke et al. (2019), clinical deterioration can go unnoticed until it necessitates higher escalation [2]. This highlights the need for more sensitive and real-time monitoring tools. Combining this with closely monitoring patients and utilising trend data, nurses can make informed decisions that could prevent clinical deterioration and potentially reduce the patient’s length of stay.
The Role of Cardiac Output Monitoring
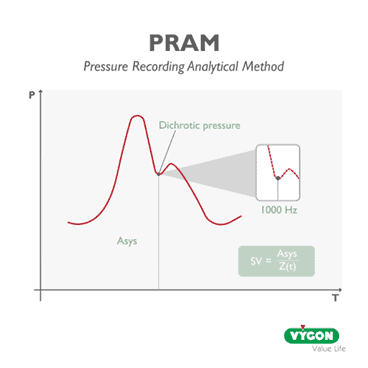
A cardiac output monitor, such as one incorporating the Pressure Recording Analytical Method (P.R.A.M), allows for constant and sensitive monitoring of haemodynamic variations in real-time. P.R.A.M. deduces the systolic output and other haemodynamic variables from analysis of the arterial pressure curve morphology alone, which it acquires accurately, sampling at a rate of 1000 Hz during each cardiac cycle, thus enabling continuous monitoring that is sensitive to the slightest haemodynamic changes in the patient.
This means that every single arterial pulse is detected and analysed; every change in the patient’s state and every reaction to a stimulus by the operator is immediately detected, analysed and provided in real time, beat by beat.
Benefits for Nursing Practice:
- Enhanced Early Detection: Continuous CO monitoring facilitates the early detection of haemodynamic changes, enabling nurses to proactively address potential issues.
- Data-Driven Decision Making: Trend data from CO monitors provides nurses with valuable information to make informed decisions regarding patient management.
- Increased Autonomy and Confidence: Access to real-time CO data empowers nurses to take initiative and make timely interventions, fostering a greater sense of autonomy and confidence in their clinical judgment.
- Facilitating Goal-Directed Therapy: CO monitoring allows clinicians to “target the therapy to the patient,” leading to more effective and personalised care. This aligns with the principles of early goal-directed therapy, which has demonstrated significant benefits in patients with severe sepsis and septic shock.
- Moving from Reactive to Proactive Care: By using continuous CO monitoring, nurses can move from a reactive approach to a proactive one, intervening before significant deterioration
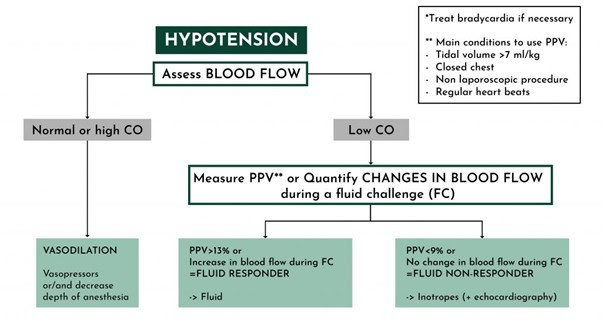
Figure 1: Rational haemodynamic management from blood pressure and blood flow monitoring. CO, cardiac output; PPV, pulse pressure variation.
Case Study: Croydon University Hospital
Croydon University Hospital in London introduced ten P.R.A.M cardiac output monitors alongside an existing nurse-led service, resulting in notable improvements. Previously, the hospital had six cardiac output machines that required calibration every 24 hours and used consumables costing around £50,000 per year. The calibration process could take up to 40 minutes per device, depending on the practitioner’s proficiency and equipment reliability.
The implementation of P.R.A.M monitors provided real-time monitoring with no complicated setup or external calibration required. This saved valuable time and eliminated consumable costs, allowing for unlimited patient care. The arterial waveform analysis cardiac output monitor enhanced the nursing team’s involvement in decisions to start or escalate/deescalate cardiac output monitoring. Previously, these decisions required approval from senior nursing or medical teams due to the associated costs.
Nurses could easily assess their patients’ needs, make necessary treatment decisions, and transfer monitoring from one patient to another. The setup was straightforward, less time-consuming, and the machine was easier to navigate, as noted by the Head of Nursing at Croydon University Hospital.
Conclusion
Cardiac output monitoring provides ICU nurses and anaesthetists with a powerful tool to enhance patient care. By enabling early detection of haemodynamic changes and supporting goal-directed therapy, nurses can make more informed decisions, leading to better patient outcomes and more efficient use of resources.
References
- McParland C, Johnston B, Cooper M. A mixed-methods systematic review of nurse-led interventions for people with multimorbidity. 2022. https://onlinelibrary.wiley.com/doi/full/10.1111/jan.15427
- Brekke IJ, Puntervoll LH, Pedersen PB, Kellett J, Brabrand M. The value of vital sign trends in predicting and monitoring clinical deterioration: A systematic review. PLoS One. 2019 Jan 15;14(1):e0210875. doi: 10.1371/journal.pone.0210875. PMID: 30645637; PMCID: PMC6333367.