At birth, neonates initiate physiological processes that facilitate their adaptation from the intrauterine environment to the extrauterine environment. This adaptation is sometimes complex due to the innumerable responses – chemical, neurological, sensory, thermal and mechanical – that a newborn must make during the first seconds of life in order to adapt adequately.
The initial moments after birth are therefore decisive in the survival of neonates, as well as the actions of healthcare professionals. Most of these patients, approximately 85%, start breathing spontaneously during the first 30 seconds of life; however, the remaining 15% may require stimulation or ventilatory support to achieve the correct transition to the new environment.
The professionals involved in care, in these first moments of life, must have the training, skills and knowledge of the appropriate procedures to act in critical situations. The development of the golden minute concept has been the imminent consequence of this context that emerges with the aim of improving survival and putting an end to prenatal deaths by offering quality and adequate care in the first 60 seconds after the birth of a newborn.
The neonatal golden minute
The golden minute strategy contemplates a logical sequence of interventions during the first minute of a newborn’s life with the aim of covering all his or her needs and facilitating his or her care. The golden minute strategy seeks to standardize a series of procedures, immediately after birth, to deal with the critical seconds for the immediate and long-term survival of the newborn.
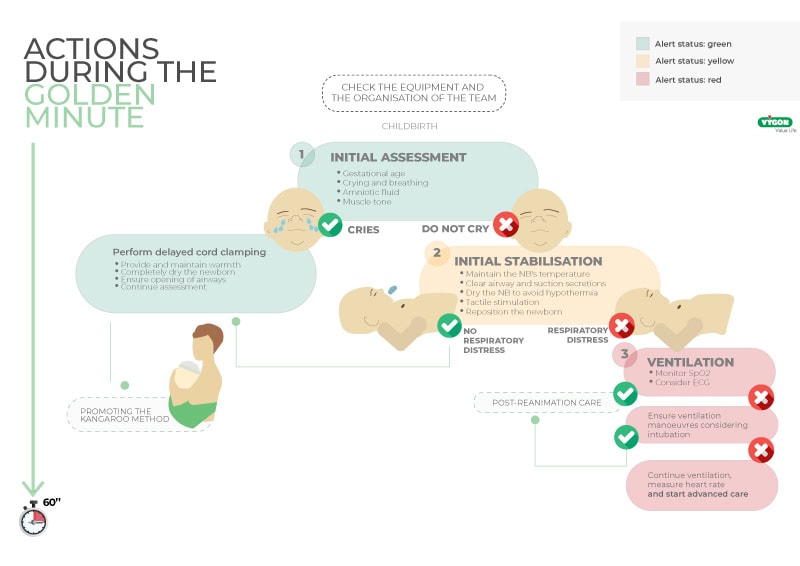
The actions planned during this minute are:
- Thermal protection of the neonate by providing warmth through a variety of strategies
- Complete drying and skin adequacy
- Suctioning of the airway in case of obstruction
- Verification of crying and breathing
- Cutting the umbilical cord
Preparation for childbirth
Before the birth takes place, it is important to verify that the appropriate area, materials and equipment are available to provide emergency care for the newborn in the event that he/she requires assistance during the first minute of life.
The professionals involved during the procedure must have the necessary skills and knowledge to carry out the care of the patient in the first minutes of life. They will also ensure that the transition between the intrauterine and extrauterine environment is as smooth as possible in order to facilitate adaptation. Thus, the room in which the delivery and subsequent interventions take place must meet three essential characteristics:
- Comply with the appropriate cleanliness and sterility requirements to avoid possible infections
- Maintain an adequate temperature to facilitate thermoregulation of the newborn and avoid hypothermia, which is common in this type of patient during the first minutes of life
- Ensure that the lighting is adapted to the needs of the professional and the newborn, taking care that the latter is not directly exposed to light, as this could cause developmental disorders
To act quickly in case of emergency, it is advisable to prepare the area and ventilation equipment in advance in case the neonate needs any kind of support to start breathing.
Initial assessment
After birth, an initial assessment of the newborn will be carried out in which the following will be evaluated:
- Gestational age and muscle tone of the newborn
- Amniotic fluid: If meconium is observed in the neonatal amniotic fluid, airway clearance is performed with determination to prevent aspiration and contact of meconium with the patient’s lungs
- Crying and breathing: another question the team of professionals should ask is whether the baby is crying. Crying is an indication that the newborn is breathing normally
Once these parameters have been checked, the newborn should be dried completely. This procedure is essential as it will help maintain the newborn’s temperature and also stimulate breathing. It is important to ensure the complete drying of the newborn and the removal of body humors since the presence of liquids in the patient’s body can facilitate cooling, even if the environmental conditions are appropriate.
Routine care
Routine care will continue for those babies who are crying, as a symptom of good health. This care consists of:
Maintaining the newborn’s body temperature
There are several valid strategies to avoid hypothermia in the neonate.
It is recommended, whenever possible, to favor the kangaroo method as a temperature control tool; also, as additional protective measures, you can use covering devices, such as plastic bags, that cover the body and head of the newborn to prevent heat loss; keep the room/room between 24ºC and 28ºC….
The latest research also indicates that in order to maintain adequate body temperature in the newborn, the first bath should be postponed.
Evaluate the newborn’s breathing
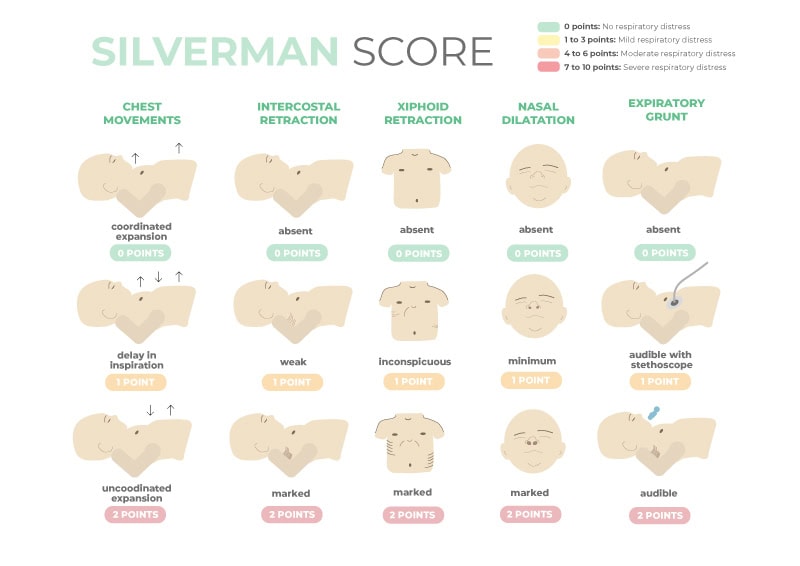
During the first seconds of the newborn’s life, the breathing of the neonate should be observed, monitoring the thoracoabdominal sounds and movement to verify that breathing is easy and calm. Tools such as the Silverman scale can be used to evaluate if there are difficulties in the patient’s breathing process:
Umbilical cord clamping
If the baby is progressing normally, delayed umbilical cord clamping is recommended. This means that the professionals will wait between 1 and 3 minutes before cutting the umbilical cord.
After establishing this care during the first minute of the newborn’s life, the professionals will continue with the normal postpartum assessment of the baby and the mother. If these requirements are met correctly, the professionals should facilitate skin-to-skin contact between mother and baby and promote breastfeeding during the first hour of life.
Stabilization
If after the first evaluation of crying and breathing the newborn is not crying or does not present a correct breathing pattern, a series of actions should be carried out with the aim of stimulating breathing:
Maintain the newborn’s body temperature
The newborn should be prevented from falling into a state of hypothermia. In this case, maintaining the kangaroo method with the mother will be complex, so other strategies should be chosen to help stabilize the temperature: use of plastic bags/devices to prevent heat loss, use of radiant cradles/incubators…
Clear the airway and remove secretions
The mouth and nose should be cleared of secretions with the appropriate suction device. It is important to follow this order, as suctioning the mouth will allow more secretions to be removed and will sometimes prevent the infant from gasping.
Repositioning the neonate
To improve the opening of the airway, the infant’s head should be positioned so that the neck is slightly extended. To ensure that the position is correct, we should check if the nose is as far forward as possible.
Tactile stimulation
Gently rubbing the back can help the onset of breathing. This stimulation should be short, as before the first minute of life the neonate should have been dried, the airway cleared and stimulated. If the infant’s respiratory pattern is still negative, ventilation should be started.
Ventilation
Before transferring the newborn to the ventilation area, previously prepared, the umbilical cord should be clamped. This procedure should be performed quickly, since delay in starting ventilation may cause short and long term complications for the newborn.
The following steps should be followed to obtain satisfactory ventilation.
Correct repositioning of the newborn
Verify correct positioning of the infant: supine position with the head in neutral position, keeping the airway open. It should allow visualization of the diaphragm movement.
Proper selection of the mask
The mask must be the appropriate size for the NB or premature infant (preferably round and transparent). It is essential to make a good seal of the nose and mouth, holding it in a C-shape with the thumb and index finger. The rest of the fingers lift the jaw in an “E” shape.

Litterature
- Ayudar a los neonatos a respirar (pp. 6–30). (2010). Amerincan Academy of Pediatrics. Recuperado de http://www.diresacusco.gob.pe/salud_individual/normas/CUADERNO%20DE%20%20ESTUDIO%20%20AYUDANDO%20A%20%20RESPIRAR%20AL%20BEBE.pdf
- Galindo , R. (2014). El minuto de oro: Ayudando a respirar a los bebés (pp. 36–38). Recuperado de https://www.uv.mx/rm/num_anteriores/revmedica_vol14_num2/articulos/el_minuto.pdf
- Girish, M. (2020). The Golden Minute after Birth – Beyond Resuscitation (p. 41). International Journal of Advanced Medical and Health Research. Recuperado de www.ijamhrjournal.org
- Moreno-Reyes, S. P. et al. (2019). Aherencia a la estrategia minuto de oro en sala de partos de una institución de segundo nivel de Cali (Colombia) (3.ª ed., pp. 155–157). Revisa Colombiana de Obstetricia y Ginecología. Revisa Colombiana de Obstetricia y Ginecología.
- Mejorar la supervivencia y el bienestar de los recién nacidos (pp. 1–3). (2020). Organización Mundial de la Salud (OMS).
- Van Heerden, C. et al. (2012). An introduction to Helping Babies Breathe: the “Golden Minute” is here for South African newborn (p. 6). Prof. Nurs Today. Prof. Nurs Today.
- Wyckoff MH, Wyllie J, Aziz K, de Almeida MF, Fabres J, Fawke J, Guinsburg R, Hosono S, Isayama T, Kapadia VS, Kim H-S, Liley HG, McKinlay CJD, Mildenhall L, Perlman JM, Rabi Y, Roehr CC, Schmölzer GM, Szyld E, Trevisanuto D, Velaphi S, Weiner GM; on behalf of the Neonatal Life Support Collaborators. Neonatal life support: 2020 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation. 2020;142(suppl 1):S185–S221. doi: 10.1161/CIR.0000000000000895





