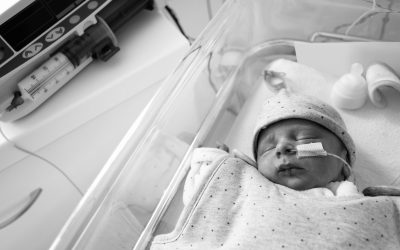
Skin lesions include MARSIs and various intrinsic or clinical conditions that pose a challenge in maintaining adequate fixation of the central catheter on the patient’s skin.
Differences between skin lesions and MARSIs
MARSIs are skin lesions due to medical adhesives: they occur only when skin comes into contact with some medical material that uses adhesives such as dressings (pictures 1 and 2), sutureless fixation systems with skin adhesion, or even electrocardiogram electrodes.
In addition, the patient may have several intrinsic and extrinsic predisposing factors such as:
- Treatment with certain drugs such as corticosteroids
- Administration of chemotherapy
- Co-morbidities such as diabetes
- Presence of previous skin problems
- Advanced or very young age.
To some extent, MARSI can be predicted and managed by following algorithms for identification, classification and treatment.
What do we know about MARSI and Vascular Access?
Increase:
- Risk of infection
- Risk of vascular access loss
- Nursing care time
- The overall cost of catheter and patient management.
Decrease:
- Patient quality of life
What do we mean with a skin lesion that is not considered as a MARSI?
When we talk about skin lesions that are generally not considered as MARSI, we refer to skin damage that may be due to different causes and not only to skin contact with adhesives used in the healthcare environment.
Since the cause of skin damage is a clinical condition or linked to intrinsic factors of the patient, its course will depend on many aspects.
It is important to note that the cause of the skin wound can sometimes be a chronic disease, such as epidermolysis bullosa, known as “butterfly skin”, which, although rare, has a genetic profile and is incurable. Other acute skin lesions can be folliculitis located on the head and neck caused by cetuximab (picture 3), burn patients or syndromes caused by Staphylococcus or other germs such as Streptococcus, which can cause acute exanthematous pustulosis (picture 4).
It is also important to consider the interference with chemical drugs and the patient’s immune system, which can lead to unusual and severe reactions (about 2% of drug reactions are considered severe). These are known as Severe Cutaneous Adverse Reactions (SCAR).
The following photo (picture 5) shows an example of a SCAR:
What is the challenge with patients with non-MARSI skin lesions?
These patients require vascular access to treat their clinical condition, or even, in the case of chronic disease, parenteral nutrition or other supportive care.
If in less severe cases, the fixation of the catheter to the skin is already a problem and means having to deal with MARSI (or the possibility of MARSI), in the population with non-MARSI skin reactions, the fixation of the venous access to the skin is a point of vital importance that can lead the health care staff to a dead end:
- How can we fix a catheter to the skin when it is not intact?
- How can we reduce skin damage that catheter fixation may cause in these patients?
- How can we ensure that a central catheter remains in place without moving to avoid repeated punctures?
If we look closely at picture 1, we can see how in order to safeguard the skin from the fixation medical adhesives, healthcare professionals have opted to fix the catheter to the skin with stitches. However, this disrupts the skin, causing a wound and making the existing problem of lack of skin integrity even worse.
Studies have long shown that suture fixation of central venous access increases the risk of infection, does not reduce the risk of leakage and is uncomfortable for the patient.
Not to mention that none of the current guidelines on vascular access recommend the use of this fixation.
At this point, we would have to look for an ideal fixation.
How can we fix vascular access catheters in these patients?
The sutureless fixation system with subcutaneous anchoring is the only device that meets these requirements and has proven its efficiency in cases of severe or rare, chronic or acute skin conditions in a hospital and home setting.
Picture 2 shows the same patient after one year with skin recovered from the MARSI that affected him and with a subcutaneous anchoring system for catheter fixation instead of sutures.
As this is a system that is attached below the epidermis, the superficial condition of the skin is not altered by its use. Moreover, in these situations, it is probably the only system that meets the ideal fixation profile in these patients.
It is advisable to use cyanoacrylate at the insertion point, which seals the exit-site in a sterile manner and provides a barrier against infections from the environment of the catheter entry point into the skin.
This way, tissue glue and subcutaneous anchoring become tools that increase the chances of central venous catheter survival in these contexts.
The subcutaneous anchor fixation system allows 360º disinfection of the skin around the catheter, without having to replace the device (since it will last as long as the catheter is in place).
It totally helps prevent trauma to the epidermis, so that superficial skin problems can be treated more easily and, presumably, with greater success (picture 6: patient with central catheter inserted centrally in the thoracic axillary vein with subcutaneous anchor fixation system and cyanoacrylate at the insertion point):
There are few references in the literature to these specific clinical situations and to the use of subcutaneous fixation for central catheters. Nonetheless, there are many experiences in several countries that align with these indications:
- Italy and the use of this system in burned patients
- Spain and the use of the system in children with butterfly skin.
Future studies in this field are necessary in order to expand knowledge about this particular aspect. As of today, it is known that this is the only device that can facilitate patient’s skin care, especially in the area where the central catheter exit is located.
If you have tried this device in any of the above situations, we would love to hear about your experience in the comments!
CONTENT USED
-
Picture 1: Patient with delicate skin due to administration of corticoids and Benadryl. Source Gloria Ortiz Miluy.
-
Picture 2: same patient as in photo 1, with subcutaneous anchorage fixation system, after one year with the same treatment. Source Gloria Ortiz Miluy.
-
Picture 3: Patient undergoing concomitant radiotherapy and chemotherapy (cetuximab) presenting acute radiodermitis together with acneiform eruption affecting the face. Source: Leal-Canosa L, Fuente- González MJ, Ribera-Pibernat M. Cutaneous side effects of antineoplastic drugs (II): kinase inhibitors and monoclonal antibodies. Skin. 2009; 24(8): 427-39.
-
Picture 4: Acute exanthematous pustulosis generalized by beta-lactams. Source: Bolte M. Severe Skin Drug Reactions. Rev Med Clin Condes. 2011; 22(6): 757-765
-
Picture 5: Toxic epidermal necrolysis due to phenytoin. Source: Bolte M. Severe Skin Skin Drug Reactions. Rev Med Clin Condes. 2011; 22(6): 757-765
-
Picture 6: Patient with rare skin condition in intensive care. Centrally inserted central catheter in thoracic axillary vein with subcutaneous anchor fixation system and cyanoacrylate at insertion point. Source: Vascular Access Team, Dr. Pittiruti.
BIBLIOGRAPHY
-
Bolte M. Severe Skin Drug Reactions. Rev Med Clin Condes. 2011; 22(6): 757-765
-
Pan RY, Chu MT, Wang CW, Lee YS, Lemonnier F, Michels AW, Schutte R, Ostrov DA, Chen CB, Phillips EJ, Mallal SA, Mockenhaupt M, Bellón T, Tassaneeyakul W, White KD, Roujeau JC, Chung WH, Hung SI. Identification of drug-specific public TCR driving severe cutaneous adverse reactions. Nat Commun. 2019 Aug 8;10(1):3569. doi: 10.1038/s41467-019-11396-2. PMID: 31395875; PMCID: PMC6687717.
-
Leal-Canosa L, Fuente- González MJ, Ribera-Pibernat M. Efectos secundarios cutáneos de los fármacos antineoplásicos (II): inhibidores de cinasas y anticuerpos monoclonales. Piel. 2009; 24(8): 427-39.
-
Fernández-Herrera J, Pedraz J. Síndrome de hipersensibilidad a fármacos. Seminarrios de la Fundación Española de Reumatología. 2007. 8(2): 55-67. DOI: 10.1016/S1577-3566(07)75604-X
-
Zhang C, Van DN, Hieu C, Craig T. Drug-induced severe cutaneous adverse reactions: Determine the cause and prevention. Ann Allergy Asthma Immunol. 2019 Nov;123(5):483-487. doi: 10.1016/j.anai.2019.08.004. Epub 2019 Aug 7. Erratum in: Ann Allergy Asthma Immunol. 2020 Apr;124(4):408. PMID: 31400461.